Cancer has been the most challenging disease that has crippled many lives and mental health. The name “cancer” itself instils fear and concern about the patient’s health and well-being. Many traditional types of treatments, such as surgery, chemotherapy, and radiation, have shown promising results. However, these treatments often leave patients with side effects. These treatments show good results with the early detection of the disease. If cancer is in a later stage or has spread to multiple organs, these treatments have less hope of fighting. Survival becomes more challenging in such advanced cases. In recent years, immunotherapy in cancer has emerged as a promising avenue for treatment. It leverages the body’s immune system to target and destroy cancer cells. Within this domain, dendritic cell therapy has gained attention as a cutting-edge strategy with the potential to revolutionise cancer treatment. In this blog, we will learn about Immunotherapy and dendritic cell therapy.
The Immune System and Dendritic Cells
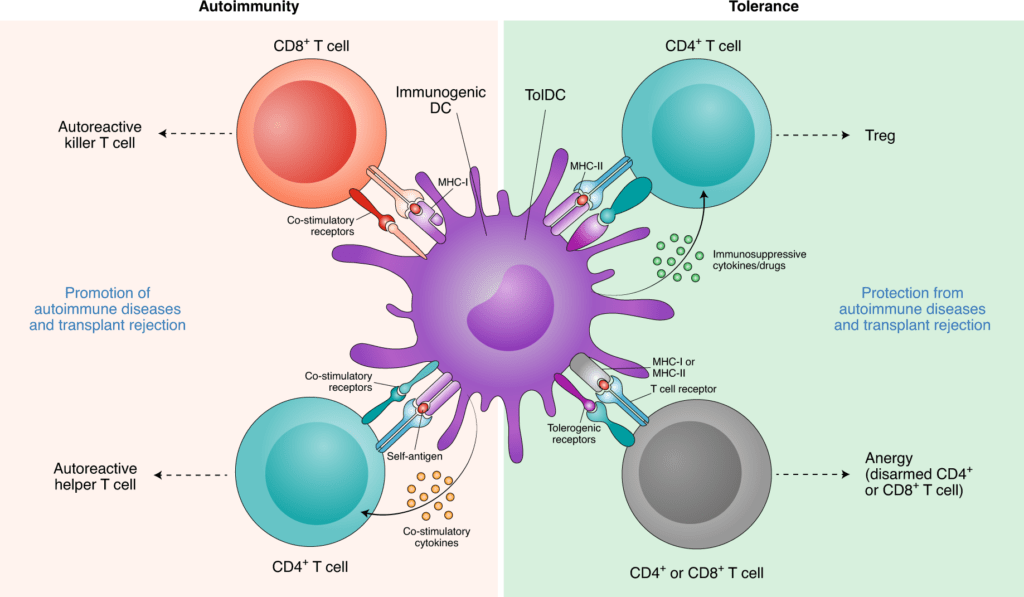
The immune system is a complex network of cells and molecules that protect the body from foreign invaders, including cancer cells. White blood cells, or leukocytes, are central to this defence mechanism, broadly categorised into two main types: the innate immune system and the adaptive immune system. Dendritic cells, often called the “sentinels” of the immune system, bridge the gap between innate and adaptive immune responses. These vigilant surveillance agents, specialized cells found throughout the body’s tissues, constantly monitor their surroundings for signs of trouble. When dendritic cells encounter foreign substances, such as pathogens or abnormal cells like cancer cells, they capture and process antigens – molecular markers specific to the invader. Dendritic cells then migrate to the lymph nodes, presenting these antigens to T cells, a type of white blood cell crucial for coordinating immune responses. Activating the adaptive immune system is crucial. It generates a targeted, specific response against the threat.
Immunotherapy for Cancer –
Immunotherapy is a revolutionary approach to cancer treatment. It offers new hope by harnessing the immune system’s power to target and destroy cancer cells. Immunotherapy represents a paradigm shift by mobilising the body’s defences to recognise and eliminate cancer cells. Our body’s immune system is a complex mix of cells, tissues, and organs. It generates defense mechanisms against foreign invaders such as infections and diseases. T cells, B cells, and natural killer (NK) cells are key players in the immune response. They collaborate to recognize and destroy abnormal cells. Cancer cells, however, can develop strategies to evade the immune system. They may produce signals that dampen immune responses or express proteins that inhibit immune cell activity. Immunotherapy for cancer aims to overcome these evasion tactics and enhance the body’s ability to recognise and attack cancer cells.
What are Dendritic Cells?
The primary function of the dendritic cell is to initiate all antigen-specific immune responses. They capture, process, and present antigens to T cells, activating the adaptive immune response. DCs act as messengers, providing essential information to other immune cells about the nature of the threat, including cancer cells.

Dendritic Cell in Immunotherapy
Immunotherapy is a broader term encompassing various strategies to improve the immune response against cancer, while dendritic cell therapy is a specific type of immunotherapy that focuses on harnessing the unique capabilities of dendritic cells.
So how does Dendritic cell therapy work?
A) Dendritic Cells as Antigen-Presenting Cells – It act as antigen-presenting cells, capturing and processing antigens from foreign substances, including cancer cells. Once loaded with these cancer-specific antigens, dendritic cells migrate to the lymph nodes, presenting the antigens to T cells and initiating a targeted immune response against the identified threat.
B) Dendritic Cell Therapy – A form of immunotherapy that involves isolating dendritic cells from a patient’s body, loading them with cancer-specific antigens, and reintroducing them into the patient. This process activates the patient’s immune system to more effectively recognise and attack cancer cells. Dendritic cells are typically harvested from a patient’s blood or bone marrow. Once isolated, they are exposed to cancer-specific antigens, which can be derived from the patient’s tumour or synthetic antigens designed to mimic those on cancer cells. This step “educates” the dendritic cells to recognise the specific characteristics of the patient’s cancer. Cells are then matured and activated in the laboratory to enhance their ability to stimulate an immune response. This maturation process primes the dendritic cells to effectively present the cancer antigens to T cells, initiating a targeted immune response. The matured and antigen-loaded dendritic cells are reintroduced into the patient. Once in the body, these educated dendritic cells present the cancer antigens to T cells, activating a specific immune response against the cancer cells. This approach aims to mobilise a more potent and targeted attack on cancer.
Final Thought –
As more advanced cell therapies are coming forward, the better future and developments we can notice. Dendritic cell therapy represents a promising frontier in the field of cancer immunotherapy. The therapy offers a targeted and potentially more effective approach to treating various malignancies by harnessing the body’s immune system and customising treatments based on individual patients and their unique cancers. In other words, one might say that it is more like a customised treatment for each patient’s cancer or tumour. Immunotherapy for cancer represents a transformative era in cancer treatment, offering new avenues for patients facing previously insurmountable odds.









